Antibiotic resistance behind 87% of typhoid economic burden: Lancet
Morning Standard
1. Key Arguments
A. AMR as the Primary Cost Driver
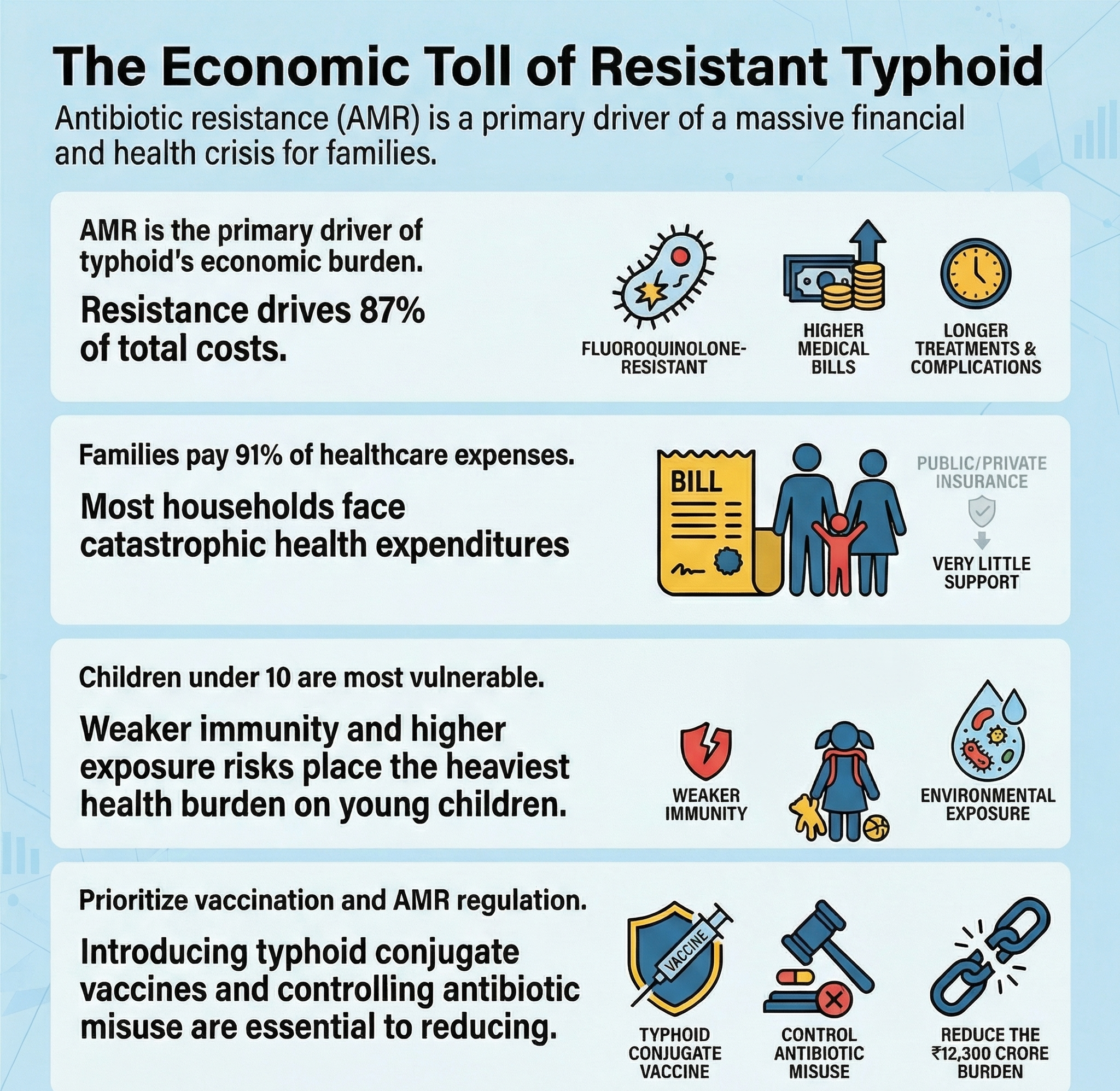
Fluoroquinolone-resistant typhoid accounts for 87% of total economic burden.
Resistance leads to longer treatment, higher costs, and greater complications.
B. High Economic Burden
Total estimated burden is substantial (~₹12,300 crore).
Includes both direct medical costs and indirect losses such as productivity.
C. Disproportionate Impact on Children
Children under 10 years bear the highest burden.
This reflects vulnerability due to weaker immunity and exposure risks.
D. Household Financial Stress
Families bear nearly 91% of healthcare expenses.
Large number of households face catastrophic health expenditure.
E. Regional Concentration of Burden
Certain states contribute disproportionately to cases and costs.
Indicates uneven healthcare access and sanitation conditions.
F. Need for Preventive Measures
Vaccination and AMR control policies are essential.
Evidence supports introduction of typhoid conjugate vaccines.
2. Author’s Stance
Evidence-based and policy-oriented
Strong emphasis on public health urgency
Highlights AMR as a critical challenge.
Support for preventive and systemic interventions
Advocates vaccination and regulatory measures.
3. Biases and Limitations
Medical-centric approach
Focuses more on treatment and resistance than broader determinants like sanitation.
Limited behavioural analysis
Antibiotic misuse patterns are not deeply explored.
Data dependency
Relies heavily on study findings without extensive contextual critique.
4. Strengths (Pros)
Data-driven insights
Grounded in credible research.
Highlights hidden economic burden
Connects health with financial impact.
Focus on vulnerable groups
Children and low-income households.
5. Weaknesses (Cons)
Limited systemic analysis
Public health infrastructure challenges need more emphasis.
Underexplored preventive ecosystem
Water, sanitation, and hygiene (WASH) factors are not deeply analysed.
Policy roadmap not fully detailed
Broad recommendations without implementation specifics.
6. Policy Implications
A. Strengthening AMR Control
Regulating antibiotic use
Prevent misuse and over-prescription.
B. Expanding Vaccination Coverage
Inclusion of typhoid vaccines in national programs
Preventive approach to reduce incidence.
C. Improving Public Health Infrastructure
Water, sanitation, and hygiene interventions
Address root causes of disease transmission.
D. Financial Protection Mechanisms
Reducing out-of-pocket expenditure
Insurance and public healthcare expansion.
E. Surveillance and Research
Monitoring resistance patterns
Data-driven policymaking.
7. Real-World Impact
Health Outcomes
Increased morbidity and mortality
Drug resistance complicates treatment.
Economic Impact
High household expenditure and poverty risk
Financial strain on families.
Public Health System
Increased burden on healthcare infrastructure
Longer treatment cycles.
Social Impact
Inequality in health access
Vulnerable groups suffer disproportionately.
8. UPSC GS Paper Linkages
GS Paper II (Governance)
- Public health policies
- Healthcare access and equity
GS Paper III (Science & Economy)
- Antimicrobial resistance
- Health economics
GS Paper I (Society)
- Vulnerability and inequality
GS Paper IV (Ethics)
- Equity in healthcare
- Responsibility in medical practice
9. Balanced Conclusion
AMR-driven typhoid burden reflects a convergence of medical, economic, and governance challenges.
While the article effectively highlights the scale of the issue, addressing it requires a comprehensive approach beyond treatment.
10. Future Perspective
From treatment to prevention
Focus on vaccination and sanitation.
Strengthening AMR governance
Regulation and awareness.
Integrated health policy
Combining medical, social, and economic interventions.
Global collaboration
AMR as a transnational challenge.
Final Insight
Antibiotic resistance is not just a medical issue—it is an economic and governance crisis that demands urgent, coordinated action.


