As AI enters healthcare, doctors grapple with safety and oversight
Indian Express
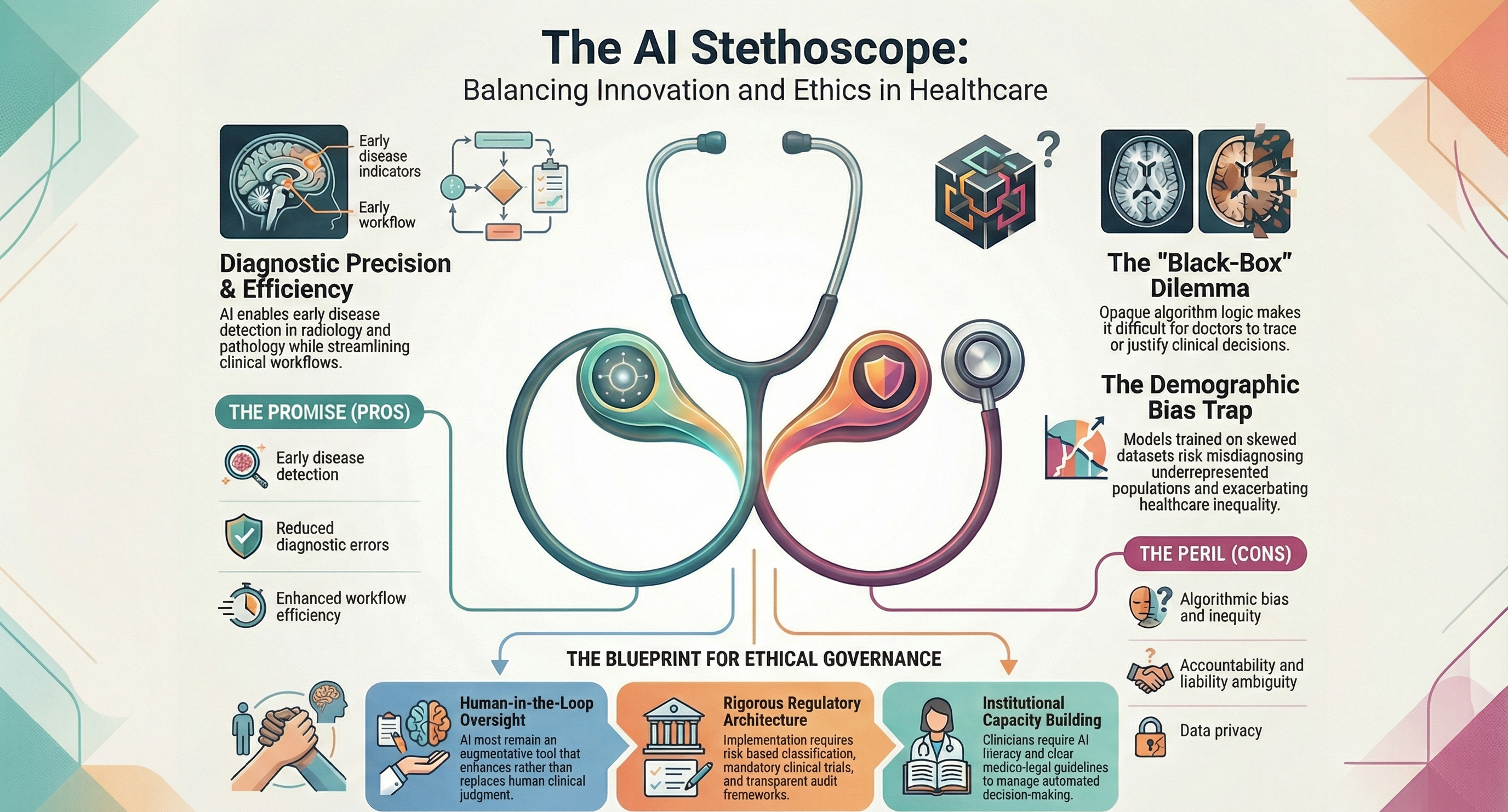
I. Core Context
The article explores the growing integration of Artificial Intelligence (AI) in healthcare, particularly in diagnostics and clinical decision-making, while highlighting concerns related to safety, bias, regulatory oversight, and accountability.
It frames AI as both:
- A transformative medical tool
- A source of ethical and governance dilemmas
II. Key Arguments Presented
1. AI’s Diagnostic Promise
The article underscores that AI can:
- Detect diseases early (e.g., radiology, pathology, ophthalmology)
- Improve efficiency in clinical workflows
- Reduce costs in the long run
- Support physicians in decision-making
AI is presented as augmentative rather than fully autonomous.
2. Data Bias and Representation Risks
A central concern raised is:
- AI models trained on limited or skewed datasets
- Underrepresentation of certain populations
- Risk of misdiagnosis due to demographic bias
Healthcare inequity may be exacerbated if datasets lack diversity.
3. Transparency and Explainability
Doctors express unease over:
- “Black-box” algorithms
- Lack of interpretability
- Difficulty in tracing decision logic
Clinical responsibility becomes complex when AI recommendations are opaque.
4. Regulatory and Oversight Gaps
The article highlights:
- Lack of clear regulatory frameworks
- Need for clinical validation
- Ethical review mechanisms
Approval processes must evolve alongside AI development.
III. Author’s Stance
The tone is balanced but cautious.
The author does not reject AI in healthcare but stresses:
- Need for rigorous oversight
- Ethical safeguards
- Clinical validation
- Human supervision
It reflects a reformist rather than alarmist perspective.
IV. Possible Biases and Limitations
1. Emphasis on Risks
While concerns are valid, the article may understate:
- Documented improvements in diagnostic accuracy
- AI’s role in rural and resource-poor settings
- Long-term cost efficiencies
2. Limited Discussion on Implementation Ecosystems
The article does not fully explore:
- Hospital readiness
- Integration with electronic health records
- Infrastructure constraints in developing countries
3. Global Regulatory Comparison Missing
The piece could have compared:
- US FDA frameworks
- EU AI Act provisions
- India’s emerging digital health policies
V. Pros and Cons of AI in Healthcare
Pros
• Early disease detection
• Reduced diagnostic error
• Enhanced workflow efficiency
• Potential cost reduction
• Expanded access in underserved regions
Cons
• Algorithmic bias
• Lack of explainability
• Accountability ambiguity
• Data privacy concerns
• Overdependence on technology
VI. Policy Implications
1. Regulatory Architecture
India must develop:
- Risk-based AI classification
- Mandatory clinical trials for AI tools
- Transparent audit frameworks
Regulation should ensure safety without stifling innovation.
2. Data Governance
Key priorities include:
- Diverse and representative datasets
- Patient consent protocols
- Data protection compliance
Bias mitigation must be institutionalised.
3. Capacity Building
Doctors require:
- AI literacy
- Interdisciplinary training
- Clear medico-legal guidelines
Human oversight remains indispensable.
4. Ethical Oversight
Institutional ethics committees should:
- Review AI deployment
- Monitor real-world outcomes
- Enforce accountability mechanisms
VII. Real-World Impact
Short-term:
- Improved diagnostic support
- Professional scepticism among clinicians
Medium-term:
- Gradual integration in radiology, oncology, cardiology
- Legal disputes over liability
Long-term:
- Transformation of healthcare delivery models
- AI-human collaborative medicine
VIII. UPSC Relevance
GS Paper II
• Health governance
• Data protection and privacy
• Regulatory institutions
GS Paper III
• Science and technology in healthcare
• Artificial Intelligence applications
• Ethical dimensions of technology
GS Paper IV
• Accountability in automated decision-making
• Ethical responsibility in public service delivery
• Human vs machine decision dilemmas
Essay Themes
• Technology and ethics
• AI and human judgment
• Innovation with responsibility
IX. Balanced Conclusion and Future Perspective
AI in healthcare is not a question of if, but how.
Its potential to revolutionise diagnostics and expand access is undeniable. Yet healthcare decisions involve life, dignity, and trust—domains that demand transparency and accountability.
The future lies in:
- Human-in-the-loop systems
- Evidence-based validation
- Robust regulatory frameworks
- Ethical data governance
AI should not replace doctors; it should enhance clinical judgment under clearly defined oversight.
Technological advancement without governance risks undermining trust. With careful design and regulation, however, AI can become a cornerstone of equitable and efficient healthcare systems.
